This gender-affirming surgery is performed under general anesthesia, ensuring the patient remains relaxed and feels no pain during the operation.
Free first visit for body and facial cosmetic surgery.
Transgender mastectomy is a gender-affirming surgery that removes breast tissue to create a flat, masculine-looking chest. This surgical procedure is indicated for transgender men and non-binary individuals seeking a body that aligns with their gender identity.
Dr. Brasó specializes in transgender mastectomy and performs this procedure using the most advanced and innovative surgical techniques. Her treatments are personalized and designed to deliver safe, natural, and harmonious results.
This gender-affirming surgery is performed under general anesthesia, ensuring the patient remains relaxed and feels no pain during the operation.
Transgender mastectomy usually takes between 2 and 3 hours.
In most cases, the patient stays one night in the hospital.
After surgery, you will wear a post-surgical compression vest and have lymphatic drainage tubes in place, which must be used daily for approximately one month.
At Clínica Brasó, we perform different mastectomy techniques for transgender patients seeking chest masculinization. The choice of technique depends on factors such as breast volume, skin elasticity, and the patient’s aesthetic goals. A specialist surgeon will evaluate each case individually to determine the most appropriate procedure.
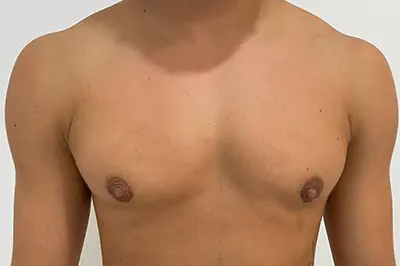
This type of mastectomy uses ultrasonic energy to simultaneously cut and coagulate breast tissue while preserving the skin and sometimes even the areola-nipple complex. It is usually recommended for patients with smaller breast volume.

Horizontal mastectomy is the traditional technique commonly used to remove breast tissue in patients with medium to large chests. This method involves making a horizontal incision beneath the chest, which may require nipple repositioning or a nipple graft afterward.
Alignment with Gender Identity
The new chest appearance achieved after surgery can reduce chest-related gender dysphoria and significantly improve overall well-being.
No more need for a binder
After surgery, compression binders are no longer necessary. Long-term binder use can cause back pain, breathing difficulties, and skin irritation.
Greater comfort and freedom of movement
The absence of breast tissue improves body posture and mobility. Physical activity becomes more comfortable, helping patients feel more confident in their bodies.
Natural and personalized results
You will achieve a more masculine and toned chest, with natural results that are harmonious with your body and gender identity.
Here are some real patient cases who have undergone transgender mastectomy at Clínica Brasó.
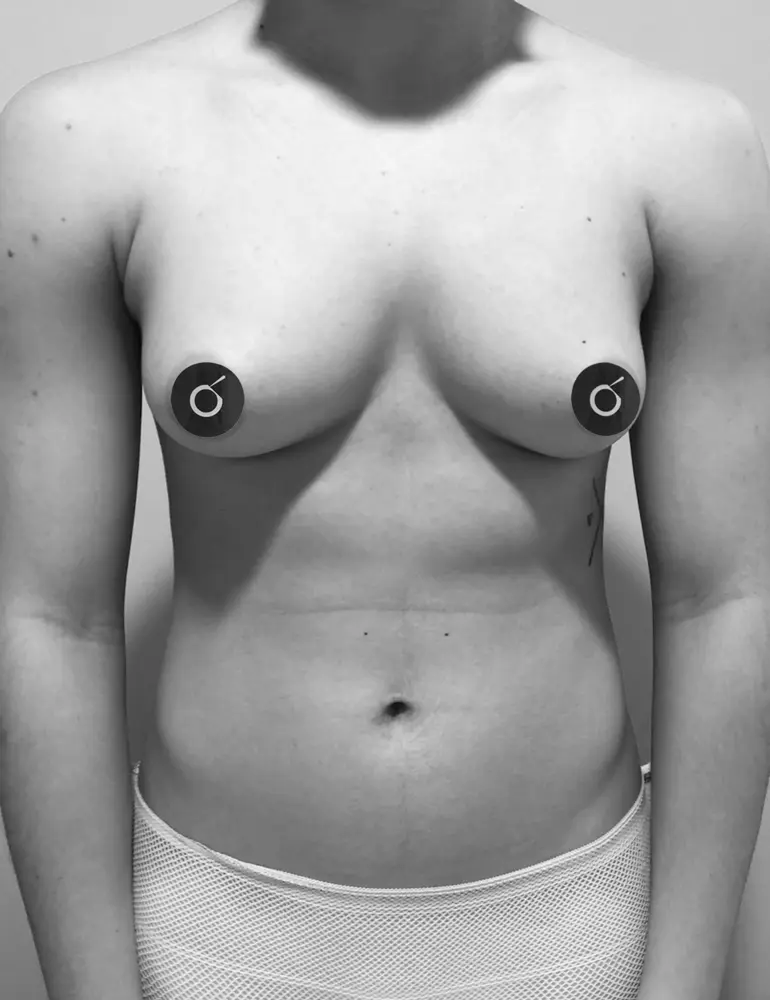
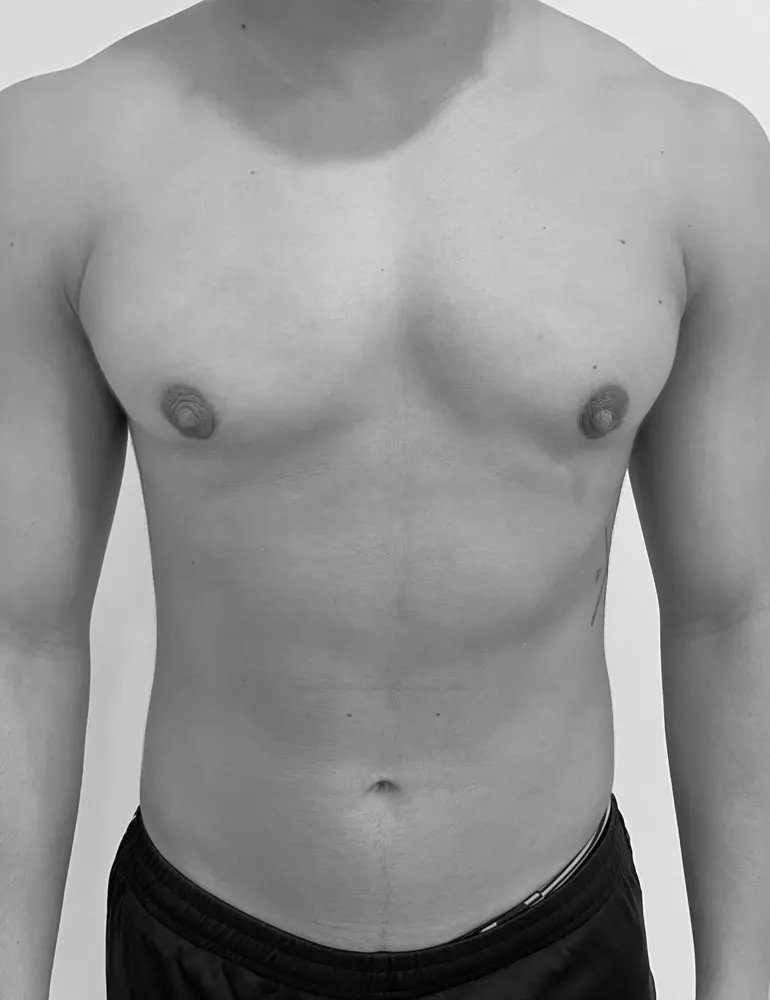
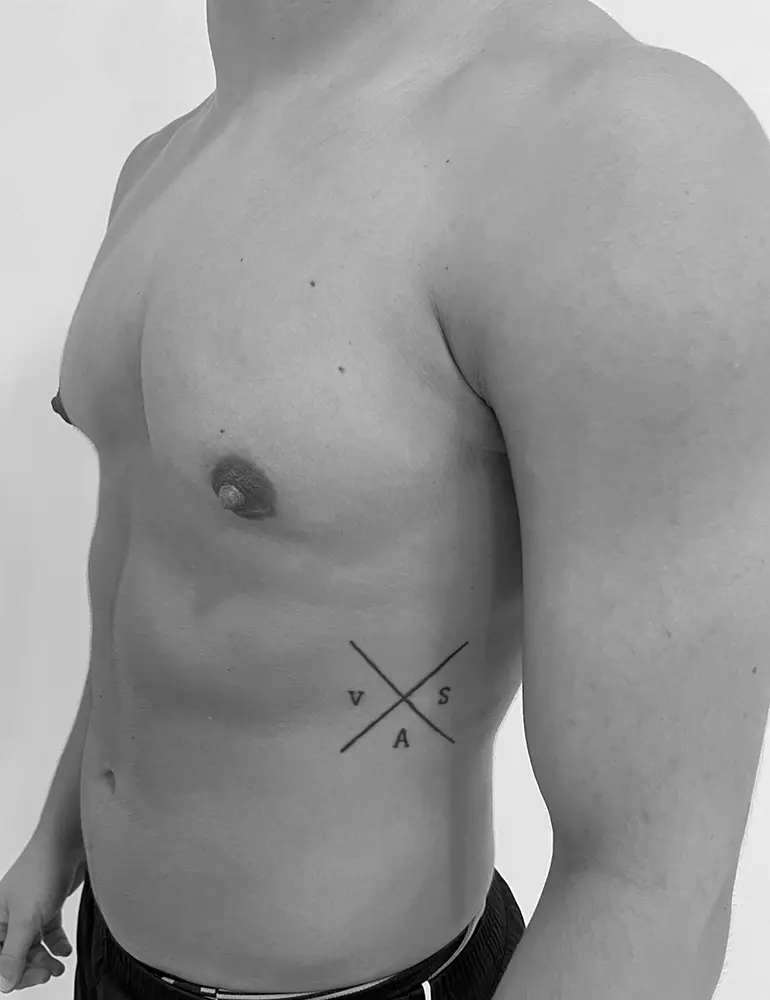
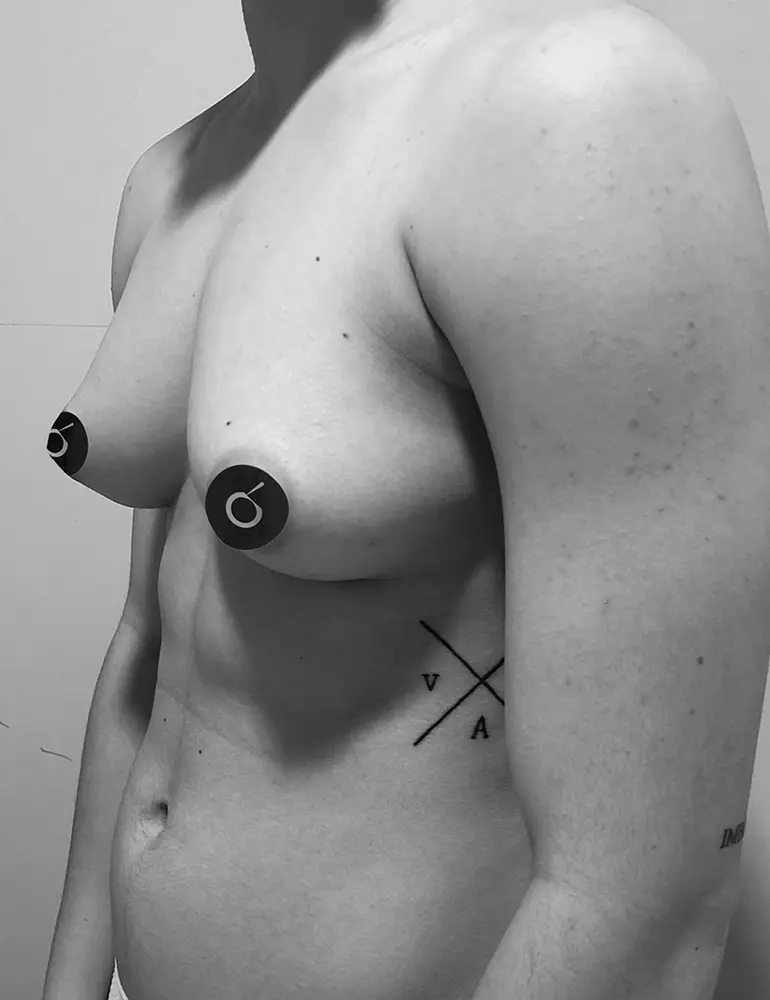
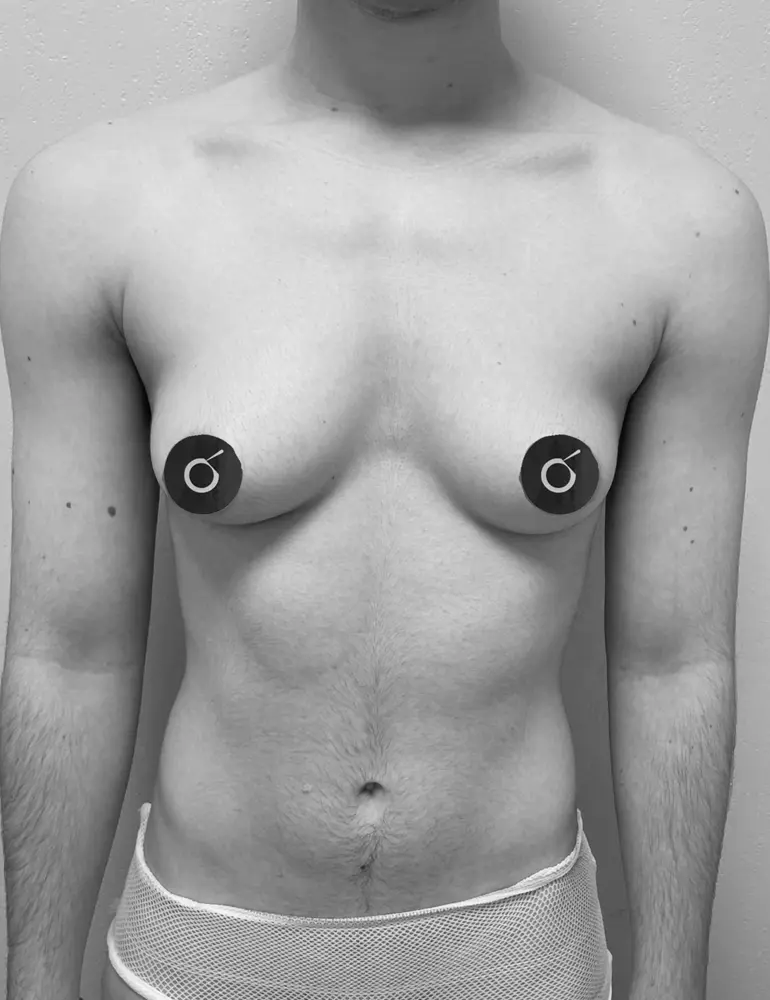
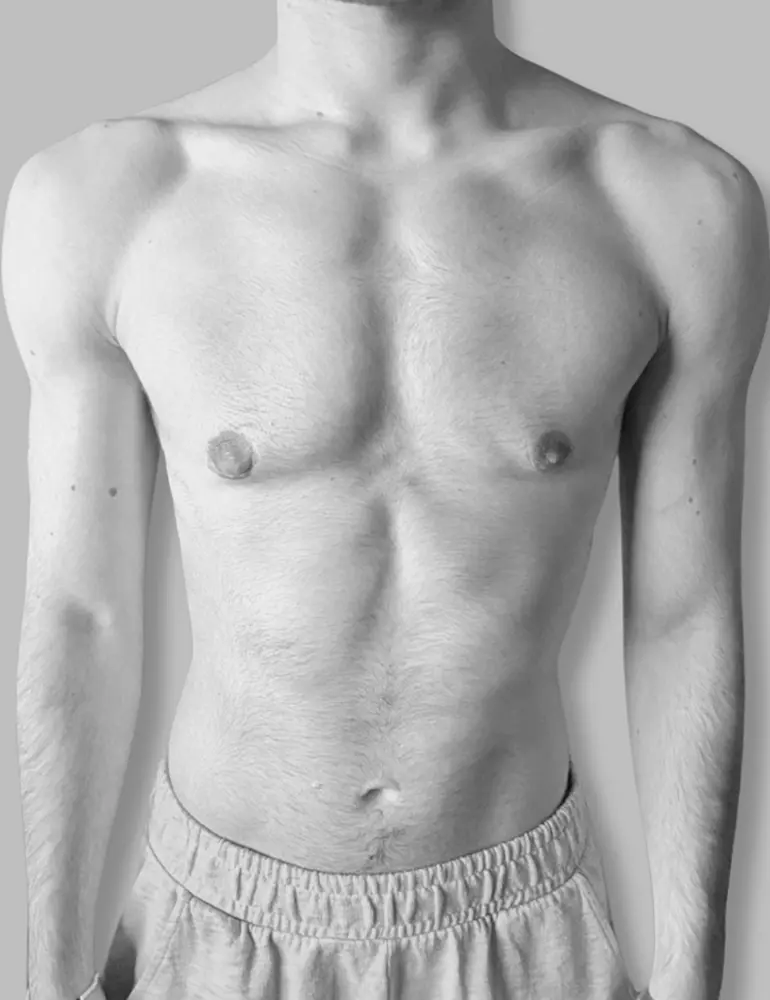
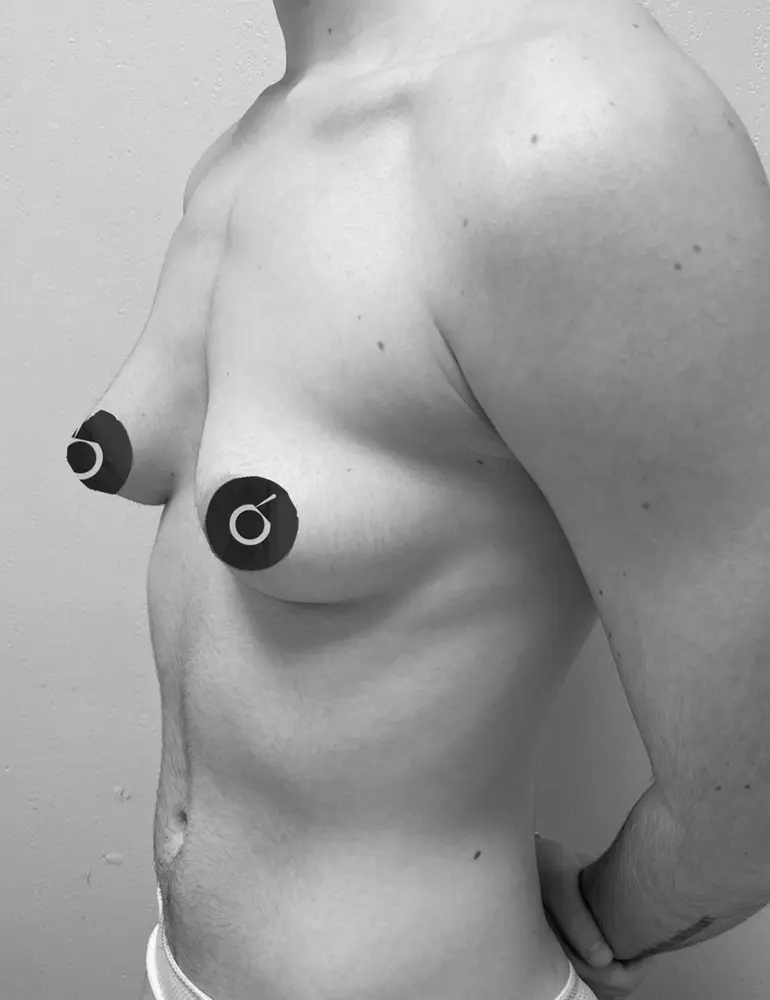

Postoperative care is essential for a safe and smooth recovery. Here’s how to take care of yourself after surgery.
Drains and compression vest
You will need to wear drainage tubes and a post-surgical compression vest for about one month to reduce swelling and help the skin adapt to the new chest contour.
Medication
During the first few days, you may experience mild discomfort or pain. Your surgeon will recommend pain relievers or anti-inflammatory medication.
Scars
It is normal for scars to appear red or swollen during the first few months. The use of silicone gels or sheets can help improve their appearance.
Sun exposure
Avoid direct sun exposure, especially during peak sunlight hours, to ensure proper healing and skin recovery.
Physical activity
You can start walking gently within a few days. Intense physical exercise should be avoided for 4 to 6 weeks.
Postoperative follow-up
After surgery, patients receive continuous medical follow-up to ensure proper healing and optimal results.
Nuestro equipo está listo para escucharte, asesorarte y guiarte en tu camino hacia tu mejor versión. No pierdas la oportunidad de dar un impulso a tu bienestar.
Responsible: UNITAT CONSULTORA DRA BRASO SLU (NIF: B56977531).
Purpose: To provide a means for you to contact us and respond to your requests for information, as well as to send communications about our products, services and activities, including by electronic means, if you check the acceptance box.
Legal basis: The user’s consent when requesting information through the contact form and by checking the acceptance box for sending information.
Data retention: Your data will be retained until your request submitted through the form is resolved or we respond via email, unless a new processing activity is required. If you have agreed to receive marketing communications, your data will be retained until you unsubscribe.
This surgery is recommended for transgender men and non-binary individuals who wish to masculinize their chest. As with any surgical procedure, medical tests and a specialist evaluation are required beforehand to assess the patient’s general health and ensure a safe intervention.
Hormone therapy is not always required. Some patients undergo testosterone therapy before surgery, but this depends on the individual case and the surgeon’s protocol.
There are several surgical techniques used for chest masculinization. The choice depends on factors such as breast size, skin elasticity, nipple-areola position, and patient expectations. The most common techniques include:
Double incision with free nipple graft – for patients with medium or large chests and low skin elasticity
Periareolar technique – for patients with smaller chests and good skin elasticity
Inverted T technique – generally recommended for patients with excess skin